General Practitioners’ Perceptions of Collaboration with Pharmacists in Primary Care Settings: A Study Driven by Social Capital Theory and Theory of Planned Behavior
DOI:
https://doi.org/10.36733/medicamento.v12i1.11141Keywords:
collaboration, general practitioner, perceptions, pharmacist, social capital theory, theory planned behaviorAbstract
Background: Pharmacists are expected to take up broader clinical roles and collaborate with general practitioners (GPs); however, data on the perception of GPs’ in the primary care settings is lacking.
Objective: This study aimed to explore GPs’ perceptions driven by Theory Planned Behavior (TPB) and Social Capital Theory (SCT) towards collaboration with pharmacists in primary care settings.
Methods: Interviews using questionnaires (with a combination of open-and closed-ended questions) were conducted with GPs at all Puskesmas in East Surabaya (n=14). Descriptive analysis was used to summarize data from closed-ended questions, and thematic analysis was used for open-ended questions.
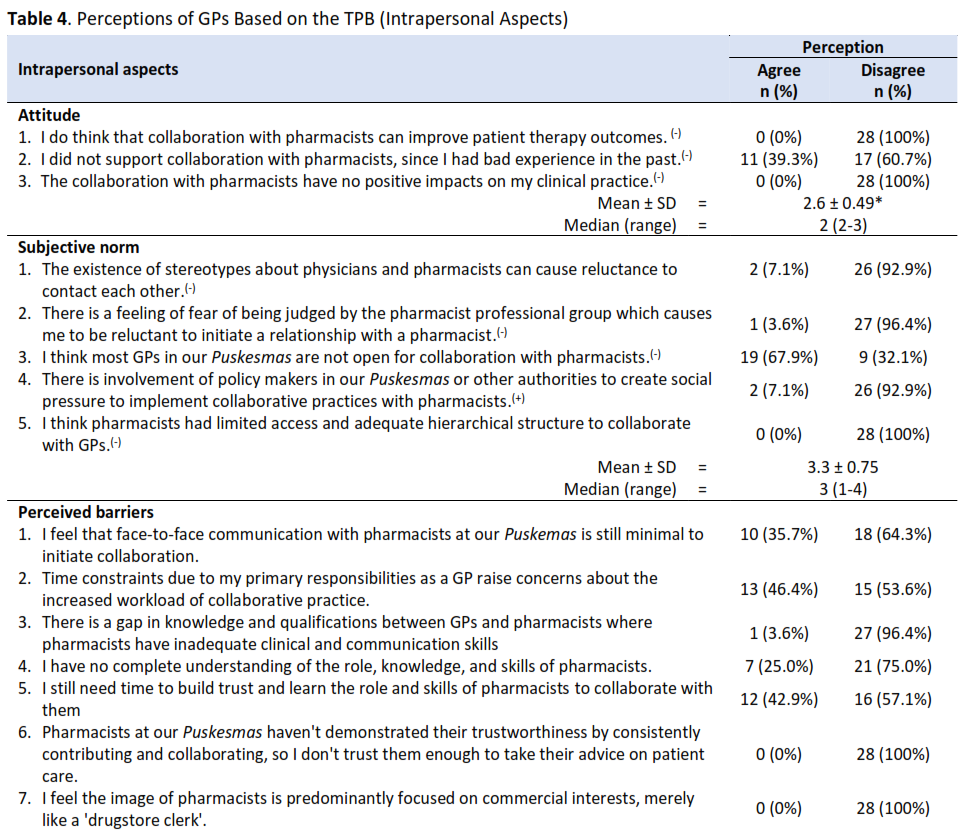
Results: A total of 28 GPs of 14 Puskesmas were included (i.e., 2 GPs per Puskesmas). The mean scores of each dimension for intrapersonal perceptions (based on TBP): 1) attitude (2.6 – positive); 2) subjective norms (3.3 – positive), 3) difficulty (2.75 – low). While the mean scores for interpersonal perceptions (based on SCT): 1) level of trust (5.7 – high); 2) level of social capital (6.0 – high). There were five themes for basic trusts: i) daily performance, ii) pharmacy skills and knowledge, iii) work experience, iv) performance track records, v) ability to communicate and collaborate with GPs. This study highlighted while GPs generally have positive perceptions, some items warrant considerations, such as negative experience with pharmacists (39.3%), lack of support from management (92.9%), and perceived difficulty to practice collaboration due to workload, cost and facilities. Additionally, 42.9% of GPs reported that they cannot fully trust delegating work to pharmacists.
Conclusions: Findings from this study should provide guidance to develop strategies to optimize collaborative practice with GPs, thus facilitating the expanded clinical roles of pharmacists in primary care settings.
References
1. Khan N, McGarry K, Naqvi AA, Holden K. Doctors’ perceptions, expectations and experience regarding the role of pharmacist in hospital settings of Pakistan. Intl J Clin Pharm. 2020;42(2):549-566. doi:10.1007/s11096-020-00991-9.
2. Albassam A, Almohammed H, Alhujaili M, Koshy S, Awad A. Perspectives of primary care physicians and pharmacists on interprofessional collaboration in Kuwait: A quantitative study. PLoS ONE. 2020;15(7):e0236114. doi:10.1371/journal.pone.0236114.
3. Sjölander M, Gustafsson M, Gallego G. Doctors’ and nurses’ perceptions of a ward-based pharmacist in rural northern Sweden. Int J Clin Pharm. 2017;39(4):953-959. doi:10.1007/s11096-017-0488-5.
4. Rayes IK, Hassali MA, Abduelkarem AR. A qualitative study exploring physicians’ perceptions on the role of community pharmacists in Dubai. Pharm Pract. 2016;14(3):738. doi:10.18549/pharmpract.2016.03.738.
5. McCutcheon L, Haines S, Valaitis R, et al. Impact of interprofessional primary care practice on patient outcomes: A scoping review. Sage Open. 2020;10(2):2158244020935899. doi:10.1177/2158244020935899.
6. Agustina R, Dartanto T, Sitompul R, et al. Universal health coverage in Indonesia: Concept, progress, and challenges. Lancet. 2019;393(10166):75-102. doi:10.1016/S0140-6736(18)31647-7.
7. Ministry of Health Republic of Indonesia (MoH-RI). Ministry of Health Regulation Number 26 in 2020: standards of pharmaceutical care in community health centres (Puskesmas) [in Indonesia]. Jakarta: MoH-RI; 2020.
8. Hasan S, Stewart K, Chapman CB, Kong DCM. Physicians’ perspectives of pharmacist-physician collaboration in the United Arab Emirates: Findings from an exploratory study. Journal of Interprofessional Care. 2018;32(5):566-574. doi:10.1080/13561820.2018.1452726
9. Lindqvist MH, Gustafsson M, Gallego G. Exploring physicians, nurses and ward-based pharmacists working relationships in a Swedish inpatient setting: a mixed methods study. International Journal of Clinical Pharmacy. 2019;41(3):728-733. doi:10.1007/s11096-019-00812-8
10. Gloria F, Pristianty L, Rahem A. Analysis of pharmacists-physicians collaboration in Surabayan community health centres from the perspectives of physisians [in Indonesian]. Jurnal Farmasi dan Ilmu Kefarmasian Indonesia. 2021;8(2):132-238. doi: 10.20473/jfiki.v8i2021.132-138.
11. Zielińska-Tomczak Ł, Cerbin-Koczorowska M, Przymuszała P, Marciniak R. How to effectively promote interprofessional collaboration? – a qualitative study on physicians’ and pharmacists’ perspectives driven by the theory of planned behavior. BMC Health Serv Res. 2021;21(1). doi:10.1186/s12913-021-06903-5
12. Li H, Huang Y, Lyu J, Xi X. The influence of social capital: a trigger for increasing job satisfaction. Psychol Res Behav Manag. 2023; 16:599-610. doi:10.2147/prbm.s402781.
13. Statistics Indonesia (Badan Pusat Statistik Republik Indonesia, BPS-RI). Populations by genders and districts/ cities across East Java Province [in Indonesia]. https://www.bps.go.id/. Accessed February 23, 2025.
14. Lestari W, Pratomoatmojo N. Spatial modeling of residential area development prediction based on Cellular Automata with a population approach in East Surabaya [in Indonesian]. Jurnal Teknik ITS. 2019;8(2):2337-9271.
15. Supper I, Catala O, Lustman M, et al. Interprofessional collaboration in primary health care: A review of facilitators and barriers perceived by involved actors. J Public Health. 2014;37(4):716-727. doi:10.1093/pubmed/fdu102.
16. DeMik DE, Weg MWV, Lundt ES, Coffey CS, Ardery G, Carter BL. Using theory to predict implementation of a physician–pharmacist collaborative intervention within a practice-based research network. Res Social Adm Pharm. 2013;9(6):719-730. doi:10.1016/j.sapharm.2013.01.003.
17. Gordon C, Unni E, Montuoro J, Ogborn DB. Community pharmacist-led clinical services: physician’s understanding, perceptions and readiness to collaborate in a Midwestern state in the United States†. Int J Pharm Pract. 2017;26(5):407-413. doi:10.1111/ijpp.12421.
18. Kelly DV, Bishop L, Young S, Hawboldt J, Phillips L, Keough TM. Pharmacist and physician views on collaborative practice. Can Pharm J/ Revue Des Pharmaciens Du Canada. 2013;146(4):218-226. doi:10.1177/1715163513492642.
19. Vinterflod C, Gustafsson M, Mattsson S, Gallego G. Physicians’ perspectives on clinical pharmacy services in Northern Sweden: a qualitative study. BMC Health Serv Res. 2018;18(1). doi:10.1186/s12913-018-2841-3
20. Jové AM, Fernández A, Hughes C, Guillén-Solà M, Rovira M, Rubio-Valera M. Perceptions of collaboration between general practitioners and community pharmacists: findings from a qualitative study based in Spain. J Interprof Care. 2014;28(4):352-357. doi:10.3109/13561820.2014.898621.
21. Bollen A, Harrison R, Aslani P, van Haastregt J. Factors influencing interprofessional collaboration between community pharmacists and general practitioners— a systematic review. Health Soc Care Community. 2019;27:e189-e212. doi:10.1111/hsc.12705.
22. Thomas J, Kumar K, Chur-Hansen A. How pharmacy and medicine students experience the power differential between professions: “Even if the pharmacist knows better, the doctor’s decision goes.” PLoS ONE. 2021;16(8):e0256776. doi:10.1371/journal.pone.0256776
23. Weissenborn M, Haefeli WE, Peters-Klimm F, Seidling HM. Interprofessional communication between community pharmacists and general practitioners: a qualitative study. Int J Clin Pharm. 2017;39(3):495-506. doi:10.1007/s11096-017-0450-6.
24. Löffler C, Koudmani C, Böhmer F, et al. Perceptions of interprofessional collaboration of general practitioners and community pharmacists - a qualitative study. BMC Health Serv Res. 2017;17(1). doi:10.1186/s12913-017-2157-8.
25. Rathbone AP, Mansoor SM, Krass I, Hamrosi K, Aslani P. Qualitative study to conceptualise a model of interprofessional collaboration between pharmacists and general practitioners to support patients’ adherence to medication. BMJ Open. 2016;6(3):e010488. doi:10.1136/bmjopen-2015-010488.
26. Gregory P, Austin Z. Trust in interprofessional collaboration. Can Pharm J/ Revue Des Pharmaciens Du Canada. 2016;149(4):236-245. doi:10.1177/1715163516647749.
27. Wilk A, Platt J. Measuring physicians’ trust: A scoping review with implications for public policy. Soc Sci Med. 2016;165:75-81. doi:10.1016/j.socscimed.2016.07.039.
28. Ansmann L, Hower KI, Wirtz MA, et al. Measuring social capital of healthcare organizations reported by employees for creating positive workplaces - validation of the SOCAPO-E instrument. BMC Health Serv Res. 2020;20(1). doi:10.1186/s12913-020-05105-9
29. Rivera-Garrido N, Ramos-Sosa MP, Accerenzi M, Brañas-Garza P. Continuous and binary sets of responses differ in the field. Sci Rep. 2022;12(1):14376. doi: 10.1038/s41598-022-17907-4.
30. Taber K. The use of Cronbach’s Alpha when developing and reporting research instruments in science education. Res Sci Educ (2018) 48:1273–1296 DOI 10.1007/s11165-016-9602-2.
31. Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77-101. doi:10.1191/1478088706qp063oa.
32. Miller R, Goodman C. Performance of retail pharmacies in low- and middle-income Asian settings: a systematic review. Health Policy Plan. 2016;31(7):940-953. doi:10.1093/heapol/czw007.
Downloads
Submitted
Accepted
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Gabby Lovarya, Yosi Irawati Wibowo, Adji Prayitno Setiadi

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.





















