The Association between Resistance of Sepsis-Inducing Bacteria to First-Line Antibiotics and Sepsis Outcome: A Retrospective Cross-Sectional Study
DOI:
https://doi.org/10.36733/medicamento.v12i1.13597Keywords:
antibiotic resistance, first-line antibiotics, sepsisAbstract
Background: Sepsis is a significant infectious disease linked to high mortality rates. Several bacterial pathogens that cause sepsis have shown resistance to first-line antibiotics. This resistance in sepsis-causing bacteria to initial antibiotic agents threatens treatment success, elevating mortality risk, healthcare costs, and prolonged hospital stays.
Objective: This study aimed to investigate the relationship between the resistance of sepsis-causing bacteria to first-line antibiotics and sepsis treatment outcomes.
Methods: This cross-sectional study was a single-center retrospective study. Data were collected from sepsis patients admitted to the intensive care unit of a general hospital in Bali between 2022 and 2023. The patients included in this study were those with a positive bacterial infection, as provided in the culture result. Therapy outcomes were evaluated based on discharge status: improved or unimproved (deceased). The resistance of sepsis-causing bacteria to first-line antibiotics, including fluoroquinolones, third- and fourth-generation cephalosporins, piperacillin-tazobactam, and vancomycin, was assessed through blood cultures. The relationship between antibiotic resistance and therapy outcomes was analyzed using the Gamma correlation coefficient. This study included 57 of 108 sepsis patients, primarily male (57.89%) and older than 60 years (57.89%).
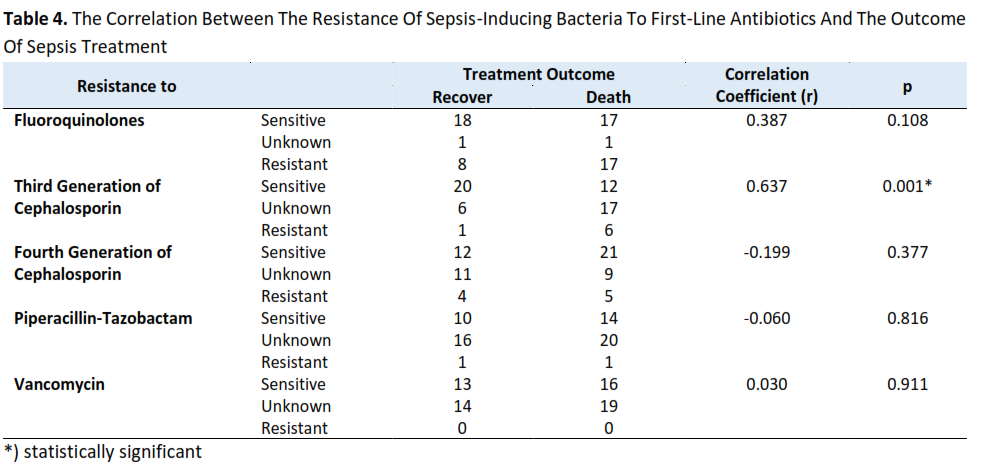
Results: A strong, significant positive correlation was observed between the resistance of sepsis-causing bacteria to third-generation cephalosporins and therapy outcomes (p=0.001; r=0.637). In contrast, resistance to fluoroquinolones (p=0.108; r=0.387), fourth-generation cephalosporins (p=0.377; r=-0.199), piperacillin-tazobactam (p=0.816; r=-0.060), and vancomycin (p=0.911; r=0.030) did not significantly impact therapy outcomes. The outcome of sepsis therapy is associated with resistance of sepsis-causing bacteria to third-generation cephalosporins but not to fluoroquinolones, fourth-generation cephalosporins, piperacillin-tazobactam, or vancomycin. This study uses a relatively small sample size, which precludes subgroup analyses.
Conclusion: Non-significant findings for some antibiotics may reflect insufficient power; further study is needed to assess the correlation between resistance of sepsis-causing bacteria to fluoroquinolones, fourth-generation cephalosporins, piperacillin-tazobactam, and vancomycin.
References
1. Fadrian F, Ahmad A, Harvindra A, Putri VY. Different Sepsis Patient Outcomes Due to Multidrug-Resistant Organisms (MDRO): A Study of Empirical Antibiotic Sensitivity Test Results. Heal Tadulako J (Jurnal Kesehat Tadulako). 2025;11(3):462-479. doi:10.22487/htj.v11i3.1740
2. Rudd KE, Johnson SC, Agesa KM, Shackelford KA, Tsoi D, Kievlan DR, Colombara D V., Ikuta KS, Kissoon N, Finfer S, Fleischmann-Struzek C, Machado FR, Reinhart KK, Rowan K, Seymour CW, Watson RS, West TE, Marinho F, Hay SI, Lozano R, Lopez AD, Angus DC, Murray CJL, Naghavi M. Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet. 2020;395(10219):200-211. doi:10.1016/S0140-6736(19)32989-7
3. Collaborators GS. Global, regional, and national sepsis incidence and mortality, 1990-2021: a systematic analysis. Lancet Glob Heal. 2025;13(12):e2013-e2026. doi:10.1016/S2214-109X(25)00356-0
4. Gretland J, Sjømæling S, Mosevoll KA, Reikvam H. Timing of antibiotic initiation in sepsis and neutropenic fever. Front Med. 2025;12(September). doi:10.3389/fmed.2025.1597047
5. Isaranuwatchai S, Buppanharun J, Thongbun T, Thavornwattana K, Harnphadungkit M, Siripongboonsitti T. Early antibiotics administration reduces mortality in sepsis patients in tertiary care hospital. BMC Infect Dis. 2025;25(1). doi:10.1186/s12879-025-10532-2
6. Strich JR, Heil EL, Masur H. Considerations for empiric antimicrobial therapy in sepsis and septic shock in an era of antimicrobial resistance. J Infect Dis. 2021;222(Suppl 2):S119-S131. doi:10.1093/INFDIS/JIAA221
7. Tićac M, Grubić Kezele T, Bubonja Šonje M. Impact of Appropriate Empirical Antibiotic Treatment on the Clinical Response of Septic Patients in Intensive Care Unit: A Single-Center Observational Study. Antibiotics. 2024;13(6):1-13. doi:10.3390/antibiotics13060569
8. Macias J, Kahly O, Edward R, Khan S, Qureshi A, Shaik A, Shala A, Shah D. Sepsis: A Systematic Review of Antibiotic Resistance and Antimicrobial Therapies. Mod Res Inflamm. 2022;11(2):9-23.
9. Marino A, Maniaci A, Lentini M, Ronsivalle S, Nunnari G, Cocuzza S, Parisi FM, Cacopardo B, Lavalle S, Via L La. The Global Burden of Multidrug-Resistant Bacteria. Published online 2025:1-20.
10. Ntambi S, Sutiningsih D, Hussein MA, Laksono B. Distribution and Prevalence of Multidrug-Resistant Organisms (MDROs) Among MDRO-Positive Individuals at Dr. Kariadi Hospital. J Epidemiol Kesehat Komunitas. 2023;8(2):103-109. doi:10.14710/jekk.v8i2.18530
11. Cornistein W, Balasini C, Nuccetelli Y, Rodriguez VM, Cudmani N, Roca MV, Sadino G, Brizuela M, Fernández A, González S, Águila D, Macchi A, Staneloni MI, Estenssoro E, Cornistein W, Balasini C, Nuccetelli Y, Rodriguez VM, Cudmani N, Roca MV, Sadino G, Brizuela M, Fernández A, González S, Águila D, Macchi A, Staneloni MI, Estenssoro E. infections in adult intensive care units in Argentina ( PREV-AR ). 2025;69(3).
12. Jalal SM, Jalal SH, Alabdullatif AA, Alasmakh KE, Alnasser ZH, Alhamdan WY. Evaluating Sepsis Management and Patient Outcomes: A Comprehensive Retrospective Study of Clinical and Treatment Data. J Clin Med. 2025;14(10):1-15. doi:10.3390/jcm14103555
13. Rhee C, Kadri SS, Dekker JP, Danner RL, Chen HC, Fram D, Zhang F, Wang R, Klompas M, Program for the CDCPE. Prevalence of Antibiotic-Resistant Pathogens in Culture-Proven Sepsis and Outcomes Associated With Inadequate and Broad-Spectrum Empiric Antibiotic Use. JAMA Netw Open. 2020;3(4):e202899-e202899. doi:10.1001/jamanetworkopen.2020.2899
14. Riccobene T, Ye G, Lock J, Yu KC, Ai CE, Gregory S, Gupta V. Outcomes of inadequate empiric therapy and timing of newer antibacterial therapy in hospitalized adults with culture-positive Enterobacterales and Pseudomonas aeruginosa: a multicenter analysis. BMC Infect Dis. 2024;24(1). doi:10.1186/s12879-024-09700-7
15. Al-Sunaidar KA, Aziz NA, Hassan Y, Jamshed S, Sekar M. Association of Multidrug Resistance Bacteria and Clinical Outcomes of Adult Patients with Sepsis in the Intensive Care Unit. Trop Med Infect Dis. 2022;7(11):1-15. doi:10.3390/tropicalmed7110365
16. Shrivastava P, Gothalwal R, Gandhi P. Therapeutic Strategies to Ameliorate Antibiotic Resistance and Host-Inflammation Response in Sepsis: an Innovative Approach. Curr Clin Microbiol Reports. 2023;10(3):85-98.
17. Debela N, Nekahiwot S. Sepsis, Antimicrobial Resistance, and Alternative Therapies. Am J Heal Res. 2024;12(1):8-18. doi:10.11648/j.ajhr.20241201.12
18. Moore DP. Battling antimicrobial resistance: new guidance and insights. Lancet Infect Dis. 2025;25(9):957-958. doi:10.1016/S1473-3099(25)00150-1
19. World Health Organnization. Global Antibiotic Resistance Surveillance Report 2025. 2025. doi:10.2471/b09585
20. Dülger D, Ture Z, Yolcu A, Eren EE, Sanlier N, Alp E. Sepsis in elderly patients: investigation of prognostic factors in a secondary healthcare facility. BMC Infect Dis. 2025;25(1). doi:10.1186/s12879-025-11286-7
21. Gabay O, Smadar-Shneyour R, Adi S, Boyko M, Binyamin Y, Novack V, Frenkel A. The Impact of Age on In-Hospital Mortality in Patients with Sepsis: Findings from a Nationwide Study. J Clin Med. 2025;14(21):1-10. doi:10.3390/jcm14217637
22. Low GKK, Harris K, Woodward M, Thompson KJ. Sex Differences in Risk Factors for Incident Sepsis Hospitalizations: A Prospective Cohort Study Using the UK Biobank. J Infect Dis. 2025;232(2):393-400. doi:10.1093/infdis/jiaf122
23. Rose N, Agrama I, Nachtigall I, Pletz MW, Rosendahl J, Chung HY, Zielinski CE, Dudziak D, Spoden M, Dröge P, Hagel S, Fleischmann-Struzek C. Sex differences in sepsis outcomes across the lifespan: a population-based cohort study in Germany. Crit Care. 2025;29(1). doi:10.1186/s13054-025-05657-4
24. Min SY, Yong HJ, Kim D. Sex or gender differences in treatment outcomes of sepsis and septic shock. Acute Crit Care. 2024;39(2):207-213. doi:10.4266/acc.2024.00591
25. Tanha N, Lejbman IA, De Bus L, De Pascale G, Garnacho-Montero J, Leone M, Fujitan S, De Waele JJ, Torisson G, Sjövall F. Clinical outcomes in combination versus mono antibiotic therapy in ICU admitted patients with a suspected infection-A substudy of the DIANA study. J Crit Care. 2024;80:154501.
26. De Bus L, Arvaniti K, Sjövall F. Empirical antimicrobials in the intensive care unit. Intensive Care Med. 2024;50(8):1338-1341. doi:10.1007/s00134-024-07453-0
27. Heffernan AJ, Sime FB, Sun J, Lipman J, Kumar A, Andrews K, Ellwood D, Grimwood K, Roberts J. β-lactam antibiotic versus combined β-lactam antibiotics and single daily dosing regimens of aminoglycosides for treating serious infections: A meta-analysis. Int J Antimicrob Agents. 2020;55(3):105839. doi:https://doi.org/10.1016/j.ijantimicag.2019.10.020
28. Strich JR, Heil EL, Masur H. Considerations for Empiric Antimicrobial Therapy in Sepsis and Septic Shock in an Era of Antimicrobial Resistance. J Infect Dis. 2020;222(Supplement_2):S119-S131. doi:10.1093/infdis/jiaa221
29. Chen X, Liu X, Ren W, Li H, Yang S. Distribution patterns and evolution of antimicrobial resistance in Gram-negative bacteria within the intensive care unit of a tertiary hospital from 2019 to 2024. Front Microbiol. 2025;16:1587132.
30. Calvo M, Stefani S, Migliorisi G. Bacterial infections in Intensive Care units: epidemiological and microbiological aspects. Antibiotics. 2024;13(3):238.
31. Trejnowska E, Deptuła A, Tarczyńska-Słomian M, Knapik P, Jankowski M, Misiewska-Kaczur A, Tamowicz B, Śmiechowicz J, Antończyk R, Armatowicz P, Sułkowski W, Durek G. Surveillance of Antibiotic Prescribing in Intensive Care Units in Poland. Can J Infect Dis Med Microbiol. 2018;2018. doi:10.1155/2018/5670238
32. Lester R, Musicha P, Van Ginneken N, Dramowski A, Hamer DH, Garner P, Feasey NA. Prevalence and outcome of bloodstream infections due to third-generation cephalosporin-resistant Enterobacteriaceae in sub-Saharan Africa: a systematic review. J Antimicrob Chemother. 2020;75(3):492-507.
33. Lester R, Musicha P, Kawaza K, Langton J, Mango J, Mangochi H, Bakali W, Pearse O, Mallewa J, Denis B, Bilima S, Gordon SB, Lalloo DG, Jewell CP, Feasey NA. Effect of resistance to third-generation cephalosporins on morbidity and mortality from bloodstream infections in Blantyre, Malawi: a prospective cohort study. The Lancet Microbe. 2022;3(12):e922-e930. doi:10.1016/S2666-5247(22)00282-8
34. Vossius G, Meex C, Moerman F, Thys M, Ernst M, Bourgeois ME, Wagner L, Delahaye T, Darcis G. Clinical Outcomes of Third-Generation Cephalosporin Definitive Therapy for Bloodstream Infections Due to Enterobacterales with Potential AmpC Induction: A Single-Center Retrospective Study. Pathogens. 2023;12(9):1152.
35. Totté JE, Quiblier C, Nolte O, Hinic V, Wunderink HF, Egli A, Mancini S. Phenotypic susceptibility profiles of AmpC-and/or extended-spectrum beta-lactamase-(co) producing Escherichia coli strains. JAC-Antimicrobial Resist. 2025;7(3):dlaf091.
36. Tebano G, Zaghi I, Cricca M, Cristini F. Antibiotic treatment of infections caused by AmpC-producing Enterobacterales. Pharmacy. 2024;12(5):142.
37. Hixon AM, Micek S, Fraser VJ, Kollef M, Guillamet MCV. Impact of Gram-Negative Bacilli Resistance Rates on Risk of Death in Septic Shock and Pneumonia. In: Open Forum Infectious Diseases. Vol 11. Oxford University Press US; 2024:ofae219.
38. Niederman MS, Baron RM, Bouadma L, Calandra T, Daneman N, DeWaele J, Kollef MH, Lipman J, Nair GB. Initial antimicrobial management of sepsis. Crit Care. 2021;25(1):307. doi:10.1186/s13054-021-03736-w
39. Aiken AM, Rehman AM, de Kraker MEA, Madrid L, Kebede M, Labi AK, Obeng-Nkrumah N, Nyamwaya B, Kagucia E, Cocker D. Mortality associated with third-generation cephalosporin resistance in Enterobacterales bloodstream infections at eight sub-Saharan African hospitals (MBIRA): a prospective cohort study. Lancet Infect Dis. 2023;23(11):1280-1290.
40. Andrade C. Sample size and its importance in research. Indian J Psychol Med. 2020;42(1):102-103.
Downloads
Submitted
Accepted
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Herleeyana Meriyani, Dwi Arymbhi Sanjaya, Rr. Asih Juanita, Nyoman Budiartha Siada, I Wayan Maysa Yudiartha, Kadek Suryawan

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.





















