Determinants of Medication Adherence Intention in Type 2 Diabetes Patients: A Theory of Planned Behavior in Javanese Society
DOI:
https://doi.org/10.36733/medicamento.v12i1.12680Keywords:
determinants, medication adherence, medication, Javanese society, type 2 diabetes mellitus.Abstract
Background: Diabetes mellitus (DM) requires long-term therapy, which may reduce patients’ adherence to medication and ultimately lead to treatment failure.
Objective: This study aimed to analyze factors influencing medication adherence intention among patients with type 2 diabetes mellitus (T2DM) based on the Theory of Planned Behavior (TPB).
Methods: An analytical observational study with a cross-sectional design was conducted among patients diagnosed with T2DM in Purworejo Regency, Central Java. Data was collected using a structured questionnaire and analyzed using binary logistic regression in SPSS version 25. A total of 382 respondents were included in the analysis.
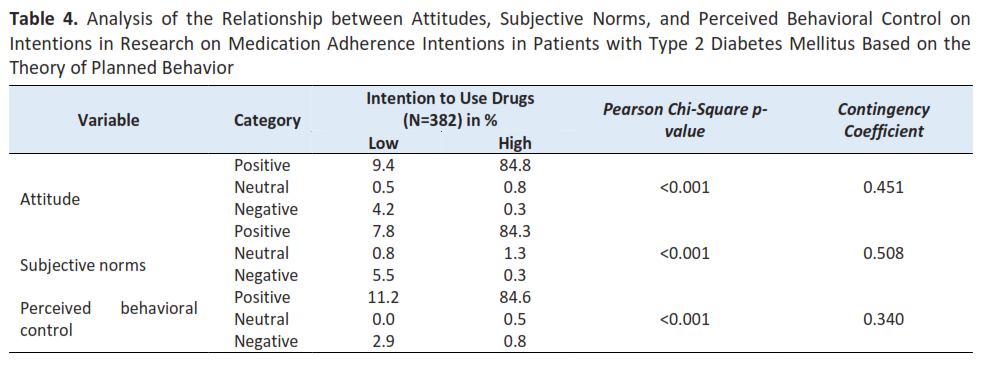
Results: Most participants were female, aged 55–65 years, employed, and had an elementary school education or equivalent. The proportion of respondents with high medication adherence intention was 85.9%. Attitude, subjective norm, and perceived behavioral control jointly explained 53.6% of the variance in medication adherence intention. Among these variables, subjective norm demonstrated the strongest association with adherence intention (OR = 197.019; p < 0.001).
Conclusion: These findings suggest that social influence, particularly encouragement and support from family members and healthcare providers, plays a dominant role in shaping medication adherence intention within a collectivist socio-cultural setting. Integrating culturally sensitive, family-centered approaches into diabetes management programs may therefore strengthen adherence intention and improve long-term treatment outcomes among patients with T2DM.
References
1. Oktora SI, Butar Butar D. Determinants of diabetes mellitus prevalence in Indonesia. J Kesehat Masy. 2022;18(2):266-273. doi:10.15294/kemas.v18i2.31880
2. Badan Penelitian dan Pengembangan Kesehatan. Laporan Riskesdas 2018 Nasional [National Riskesdas Report 2018]. Jakarta: Lembaga Penerbit Balitbangkes; 2019:70-75. https://repository.badankebijakan.kemkes.go.id/id/eprint/3514/1/Laporan Riskesdas 2018 Nasional.pdf
3. American Diabetes Association. Standards of medical care in diabetes—2016 abridged for primary care providers. Clin Diabetes. 2016;34(1):3-21. doi:10.2337/diaclin.34.1.3
4. Davies MJ, D’Alessio DA, Fradkin J, Kernan WN, Mathieu C, Mingrone G, Rossing P, Tsapas A, Wexler DJ, Buse JB. Management of hyperglycemia in type 2 diabetes, 2018: a consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2018;41(12):2669-2701. doi:10.2337/dci18-0033
5. Davies MJ, Aroda VR, Collins BS, Gabbay RA, Green J, Maruthur NM, Rosas SE, Del Prato S, Mathieu C, Mingrone G, Rossing P, Tsapas A, Buse JB. Management of hyperglycemia in type 2 diabetes, 2022: a consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2022;45(11):2753-2786. doi:10.2337/dci22-0034
6. Dal Canto E, Ceriello A, Rydén L, Ferrini M, Hansen TB, Schnell O, Standl E, Beulens JWJ. Diabetes as a cardiovascular risk factor: an overview of global trends of macro and microvascular complications. Eur J Prev Cardiol. 2019;26(2 suppl):25-32. doi:10.1177/2047487319878371
7. Mohebi S, Parham M, Sharifirad G, Gharlipour Z. Social support and self-care behavior study. J Educ Health Promot. 2018;7:1-6. doi:10.4103/jehp.jehp
8. Polonsky WH, Henry RR. Poor medication adherence in type 2 diabetes: recognizing the scope of the problem and its key contributors. Patient Prefer Adherence. 2016;10:1299-1306. doi:10.2147/PPA.S106821
9. Ekpor E, Osei E, Akyirem S. Prevalence and predictors of traditional medicine use among persons with diabetes in Africa: a systematic review. Int Health. 2024;16(3):252-260. doi:10.1093/inthealth/ihad080
10. Hertroijs DFL, Elissen AMJ, Brouwers MCGJ, Hiligsmann M, Schaper NC, Ruwaard D. Preferences of people with type 2 diabetes for diabetes care: a discrete choice experiment. Diabet Med. 2020;37(11):1807-1815. doi:10.1111/dme.13969
11. Liu H, Yao Z, Shi S, Zheng F, Li X, Zhong Z. The mediating effect of self-efficacy on the relationship between medication literacy and medication adherence among patients with type 2 diabetes. Patient Prefer Adherence. 2023;17:1657-1670. doi:10.2147/PPA.S413385
12. Sahoo J, Mohanty S, Kundu A, Epari V. Medication adherence among patients of type II diabetes mellitus and its associated risk factors: a cross-sectional study in a tertiary care hospital of Eastern India. Cureus. 2022;14(12):e33074. doi:10.7759/cureus.33074
13. Alfian SD, Sukandar H, Lestari K, Abdulah R. Medication adherence contributes to an improved quality of life in type 2 diabetes mellitus patients: a cross-sectional study. Diabetes Ther. 2016;7(4):755-764. doi:10.1007/s13300-016-0203-x
14. Dilekler İ, Doğulu C, Bozo Ö. A test of theory of planned behavior in type II diabetes adherence: the leading role of perceived behavioral control. Curr Psychol. 2021;40(7):3546-3555. doi:10.1007/s12144-019-00309-7
15. Hsu SH, Tang KP, Lin CH, Chen PC, Wang LH. Applying the theory of planned behavior to investigate type 2 diabetes patients’ intention to receive injection therapy. Front Public Health. 2023;11:1066633. doi:10.3389/fpubh.2023.1066633
16. Fles R, Bos ACRK, Supriyati, Rachmawati D, Waliyanti E, Tan IB, Haryanna SM, Schmidt MK, Dewi FST. The role of Indonesian patients' health behaviors in delaying the diagnosis of nasopharyngeal carcinoma. BMC Public Health. 2017;17(1):510. doi:10.1186/s12889-017-4429-y
17. Permana I, Ormandy P, Ahmed A. Maintaining harmony: how religion and culture are interwoven in managing daily diabetes self-care. J Relig Health. 2019;58(4):1415-1428. doi:10.1007/s10943-019-00819-5
18. Sari Y, Yusuf S, Haryanto, Hidayat AA, Rachmawati IN. The cultural beliefs and practices of diabetes self-management in Javanese diabetic patients: an ethnographic study. Heliyon. 2022;8(2):e08873. doi:10.1016/j.heliyon.2022.e08873
19. Pan L, Zhang X, Wang S, Zhang X, Li H, Wang Y. Determinants associated with self-management behavior among type 2 diabetes patients in China: a structural equation model based on the theory of planned behavior. Int J Clin Health Psychol. 2023;23(1):100332. doi:10.1016/j.ijchp.2022.100332
20. Prihandiwati E, Rahem A, Rachmawati. Pengaruh brief counseling terhadap kepatuhan minum obat dan kadar gula darah pasien diabetes mellitus tipe II di RSUD Ulin Banjarmasin [Effect of brief counseling on medication adherence and blood glucose levels in type II diabetes mellitus patients at Ulin Hospital Banjarmasin]. J Ilm Mhs Univ Surabaya. 2018;7(1):2068-2085.
21. Rezaei M, Valiee S, Tahan M, Ebtekar F, Ghanei Gheshlagh R. Barriers of medication adherence in patients with type 2 diabetes: a pilot qualitative study. Diabetes Metab Syndr Obes. 2019;12:589-599. doi:10.2147/DMSO.S197159
22. Pratiwi FI, Widayati A. Pengaruh intervensi tenaga kesehatan terhadap kepatuhan minum obat pada pasien diabetes mellitus tipe 2 di Indonesia: kajian literatur [Effect of healthcare professional interventions on medication adherence in patients with type 2 diabetes mellitus in Indonesia: a literature review]. J Sains Farm Klin. 2021;8(2):107-115. doi:10.25077/jsfk.8.2.107-115.2021
23. Lestarina NNW. Theory of planned behavior sebagai upaya peningkatan kepatuhan pada klien diabetes melitus [Theory of planned behavior as an effort to improve adherence among diabetes mellitus patients]. Media Kesehat Masy Indones. 2018;14(2):201-210. doi:10.30597/mkmi.v14i2.3987
24. Wu P, Liu N. Association between patients’ beliefs and oral antidiabetic medication adherence in a Chinese type 2 diabetic population. Patient Prefer Adherence. 2016;10:1161-1167. doi:10.2147/PPA.S105600
25. Kusumo MP, Hendrartini J, Sufro ZM, Dewi FST. A qualitative study to explore the perception of patients towards diet in Javanese culture. Enferm Clin. 2020;30:183-187. doi:10.1016/j.enfcli.2020.06.041
26. Nurlatif RV, Sumardiyono S, Rahardjo SS. Prevention and control of diabetes mellitus complications in productive population in rural areas. Int J Public Health Sci. 2024;13(1):50-58. doi:10.11591/ijphs.v13i1.23424
27. Widayanti AW, Green JA, Heydon S, Norris P. Health-seeking behavior of people in Indonesia: a narrative review. J Epidemiol Glob Health. 2020;10(1):6-15. doi:10.2991/jegh.k.200102.001
28. Qin Z, Zhou K, Li Y, Li X, Li S, Zhao X. The atherogenic index of plasma plays an important role in predicting the prognosis of type 2 diabetic subjects undergoing percutaneous coronary intervention: results from an observational cohort study in China. Cardiovasc Diabetol. 2020;19(1):1-11. doi:10.1186/s12933-020-0989-8
29. Aschner P. New IDF clinical practice recommendations for managing type 2 diabetes in primary care. Diabetes Res Clin Pract. 2017;132:169-170. doi:10.1016/j.diabres.2017.09.002
30. Guénette L, Breton MC, Guillaumie L, Lauzier S, Grégoire JP, Moisan J. Psychosocial factors associated with adherence to non-insulin antidiabetes treatments. J Diabetes Complications. 2016;30(2):335-342. doi:10.1016/j.jdiacomp.2015.10.016
31. Nanda OD, Wiryanto B, Triyono EA. Hubungan kepatuhan minum obat anti diabetik dengan regulasi kadar gula darah pada pasien perempuan diabetes mellitus [Relationship between adherence to antidiabetic medication and blood glucose regulation in female diabetes mellitus patients]. Amerta Nutr. 2018;2(4):340-348. doi:10.20473/amnt.v2i4.2018.340-348
32. Ehwarieme TA, Ogbogu CJ, Mbadugha C, Obiekwu AL. Compliance to treatment regimen among diabetic patients attending outpatient department of selected hospitals in Benin City, Edo State. J Public Health Epidemiol. 2018;10(4):97-107. doi:10.5897/jphe2018.1002
33. Oktaviani B, Widagdo L, Widjanarko B. Faktor yang berhubungan dengan kepatuhan penderita diabetes mellitus dalam menjalani pengobatan di Puskesmas Pudak Payung Kota Semarang [Factors associated with treatment adherence among diabetes mellitus patients at Pudak Payung Primary Health Center, Semarang]. J Kesehat Masy. 2018;6:2356-3346.
34. Ghassab-Abdollahi N, Nadrian H, Pishbin K, Shirzadi S, Sarbakhsh P, Saadati F, Moradi MS, Sefidmooye Azar P, Zhianfar L. Gender and urban–rural residency-based differences in the prevalence of type 2 diabetes mellitus and its determinants among adults in Naghadeh: results of the IraPEN survey. PLoS One. 2023;18(3):e0279872. doi:10.1371/journal.pone.0279872
35. Endrias EE, Feleke MG. Magnitude of high body mass index and its associated factors among adult type 2 diabetes mellitus patients attending follow-up clinics at hospitals in Wolaita Zone, Southern Ethiopia, 2021. Int J Afr Nurs Sci. 2023;19:100579. doi:10.1016/j.ijans.2023.100579
36. Zhao Q, Laukkanen JA, Li Q, Li G. Body mass index is associated with type 2 diabetes mellitus in Chinese elderly. Clin Interv Aging. 2017;12:745-752. doi:10.2147/CIA.S130014
37. Nusantara AF, Wahyuningsih AS. Kepatuhan Pengobatan Diabetes Mellitus Tipe 2 Ditinjau Dari Karakteristik Penderita Di Desa Satrean Maron Probolinggo [Treatment adherence in type 2 diabetes mellitus based on patient characteristics in Satrean Village, Probolinggo]. Profesi (Profesional Islam Media Publ Penelit. 2019;16(2):27. doi:10.26576/profesi.310
38. Diantari IAPM, Sutarga IM. Kepatuhan minum obat pada pasien diabetes melitus tipe 2 di wilayah kerja Puskesmas Tabanan II tahun 2019 [Medication adherence among type 2 diabetes mellitus patients in the working area of Tabanan II Primary Health Center in 2019]. Arch Community Health. 2019;6(2):40-46. doi:10.24843/ach.2019.v06.i02.p04
39. Moraes NM, Souza GFP, Brito FI, Pereira EBF, Nogueira LT, Carvalho MMB. Knowledge about diabetes mellitus and self-care activities before and after an educational program: a pilot study. Open J Nurs. 2020;10(2):101-116. doi:10.4236/ojn.2020.102006
40. Rasdianah N, Martodiharjo S, Andayani TM, Hakim L. The description of medication adherence for patients with type 2 diabetes mellitus in a public health center in Yogyakarta. Indones J Clin Pharm. 2016;5(4):249-257. doi:10.15416/ijcp.2016.5.4.249
41. Ainni AN. Studi Kepatuhan Penggunaan Obat Pada Pasien Diabetes Melitus Tipe-2 di Instalasi Rawat Jalan RSUD Dr. Tjitrowardojo Purworejo Tahun 2017 [Study of medication adherence among type 2 diabetes mellitus patients in the outpatient department of Dr. Tjitrowardojo Hospital, Purworejo, 2017]. Fak Farm Univ Muhammadiyah Surakarta. Published online 2017:1-10.
42. Jasmine NS, Wahyuningsih S, Thadeus MS. Analisis faktor tingkat kepatuhan minum obat pasien diabetes melitus di Puskesmas Pancoran Mas periode Maret–April 2019 [Analysis of factors influencing medication adherence among diabetes mellitus patients at Pancoran Mas Primary Health Center, March–April 2019]. J Manaj Kesehat Indones. 2020;8(1):61-66. doi:10.14710/jmki.8.1.2020.61-66
43. Bin Rakhis SA, AlDuwayhis NM, Aleid N, AlBarrak AN, Aloraini AA. Glycemic control for type 2 diabetes mellitus patients: a systematic review. Cureus. 2022;14(6):e26180. doi:10.7759/cureus.26180
44. Chowdhury S, Chakraborty PP. Universal health coverage—there is more to it than meets the eye. J Fam Med Prim Care. 2017;6(2):169-170. doi:10.4103/jfmpc.jfmpc
45. Muthuri RNDK, Senkubuge F, Hongoro C. Senior managers’ experience with health, happiness, and motivation in hospitals and the perceived impact on health systems: the case of Meru County, Kenya. Healthc. 2021;9(3):350. doi:10.3390/healthcare9030350
Downloads
Submitted
Accepted
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Fransiska Indah Pratiwi, Aris Widayati, Pramitha Esha Nirmala Dewi

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.





















